Betty’s facelift
Meet Betty the lovely Bassett Hound. Betty is 3 years of age and as you can see from the photog..
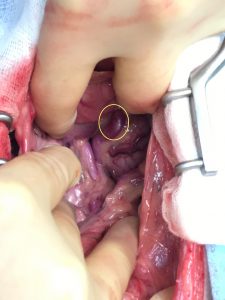
+ Read moreBobby had always been a playful kitten, but tired more easily than his brother and was prone to tummy upsets. A thorough investigation at North Wales Referrals, Buckley revealed an abnormal blood vessel – a vessel shunting blood from the stomach straight back into the venous system, without being detoxified by the liver. A liver shunt or portosystemic shunt PSS can have profound effects on a patient during its life time, causing intermittent poor appetite, periods of vomiting / diarrhoea, poor weight gain, formation of bladder stones and for some more severely affected seizures. The majority of cats and dogs with this condition are diagnosed as kittens and puppies, but there are however, some patients that are diagnosed much later in life as their shunting vessels are less impacting.
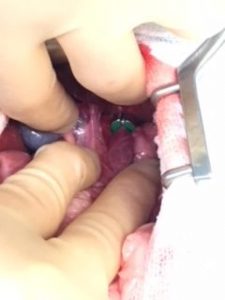
The treatment options for an extra hepatic PSS are to either give longterm medical support coupled with a balanced protein diet (not necessarily protein restricted in juvenile patients) or to perform surgery with the aim of identifying the abnormal vessel and usually applying a slow occlusion device such as a cellophane band or ameriod constrictor. An ameroid constrictor is a light weight metal ring containing casein, a product which slowly swells once it comes into contact with body fluid / moisture. Ideally, an ameroid should slowly occlude a PSS over a 6-8 week period and remains within the body, around the PSS for the patients life time. The aim of surgery is for the liver to slowly get used to the new blood volume and pressure as the PSS is closing down. A more normal blood flow through the liver, enables the liver to function more normally and ultimately for patients to be rid of their clinical signs.
Bobby’s PSS was a large vessel located in front of the stomach as depicted by ultrasound. Careful dissection around the PSS enabled a 3.5mm ameroid constrictor to be placed. Bobby recovered well and I am pleased to report did not develop any neurological signs during the first week following surgery. In approximately 5% of patients, during the first 7 days, a potentially fatal neurological syndrome can develop and we may not be able to control these signs. Bobby’s owners were very vigilant looking out for signs such as tremors, ataxic/ wobbling/ inappropriate vocalising/ seizures. None developed, and Bobby continues to thrive and grow.